Your cholesterol is normal. Your blood pressure is fine. But calcium quietly building up in your arteries tells a different story. There’s a scan for that — do you need it?
What Is a Coronary Artery Calcium (CAC) Scan?
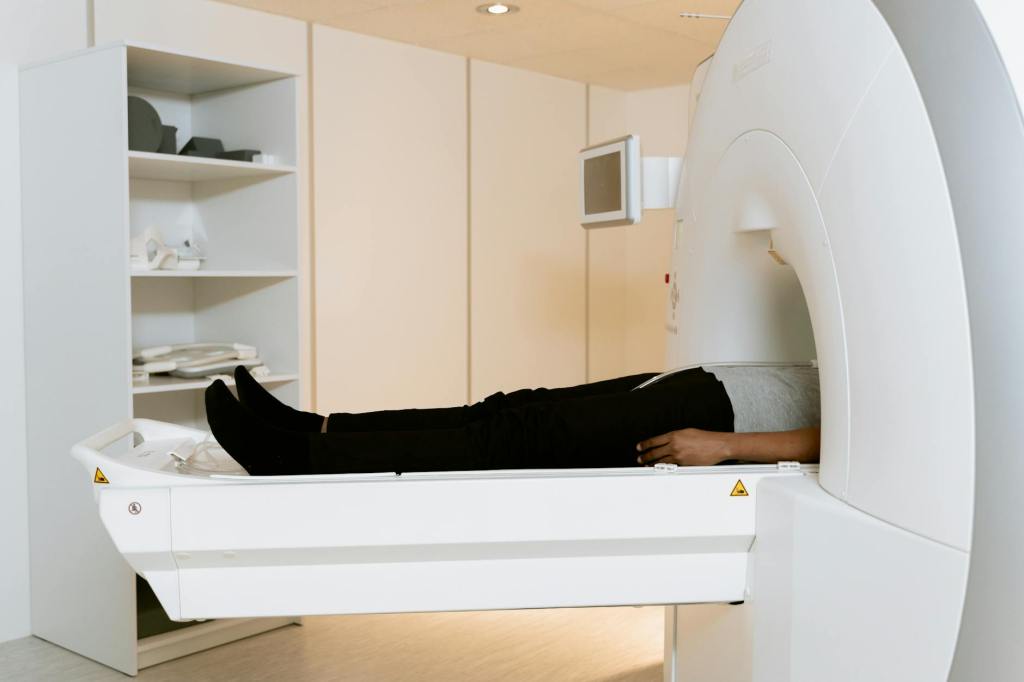
A CAC scan is a non-invasive CT scan that detects calcium deposits in the walls of the arteries that supply your heart. These deposits — called calcified plaques — are a hallmark of atherosclerosis, the gradual hardening and narrowing of arteries that can lead to heart attacks.
The result is expressed as a CAC score, which ranges from zero upward. A score of zero means no calcification was detected. Scores above 100 or 300 signal progressively higher levels of plaque buildup.
Importantly, this test is for people with no heart disease symptoms. It’s a preventive screening tool, not a diagnostic one.
Who Is It For?
The American College of Cardiology and American Heart Association (ACC/AHA) recommend considering a CAC scan for specific groups.
The clearest candidates are adults aged 40 to 75 who fall into an “intermediate risk” category, meaning their estimated 10-year risk of a major cardiovascular event is between 7.5% and 20%. For these patients, traditional risk calculators (which factor in age, cholesterol, blood pressure, and smoking status) may leave the treatment decision — particularly around starting statin therapy — genuinely uncertain. The CAC score can break that tie.
The guidelines also support CAC testing for adults in a “borderline risk” category (5%–7.5% 10-year risk) if they have additional risk-enhancing factors, such as:
- A family history of premature heart disease
- Persistently elevated LDL cholesterol (≥160 mg/dL) or triglycerides (≥175 mg/dL)
- Chronic kidney disease
- Metabolic syndrome
- Inflammatory conditions like rheumatoid arthritis, psoriasis, or HIV
- Pregnancy-related complications such as preeclampsia, or premature menopause
- South Asian ancestry, which is associated with higher cardiovascular risk
In certain cases, younger adults under 40 with a strong family history of early heart disease may also benefit — though calcified plaque is uncommon in this age group and careful clinical judgment is needed.
To learn more about calculating your risk, click here.
What Do the Scores Mean?
Once you have a CAC score, here’s how it generally translates into action:
CAC = 0: Your risk of a cardiovascular event in the next five years is very low. Statin therapy can likely be deferred, and your doctor may recommend a repeat scan in five years if you’re over 40.
CAC 1–99: There is some plaque present. Statin therapy may be worth considering, particularly for younger patients or those with other risk factors.
CAC 100–299: You are clearly in statin-eligible territory. Your risk of a major event is estimated at 7.5% to 20% over ten years.
CAC ≥ 300: This signals high risk. High-intensity statin therapy is typically recommended at this threshold.
One important nuance: a CAC score of zero doesn’t guarantee you have no arterial plaque — it just means there is no calcified plaque. Non-calcified plaques can still exist but won’t be detected by this test.
Who Should NOT Get a CAC Scan?
The test is not for everyone, and clinical guidelines are clear about when it adds little value:
- People already taking a statin — the result won’t change their treatment
- Those with known heart disease (prior heart attack, bypass surgery, or stent placement)
- Patients with diabetes, current smokers, or those with familial hypercholesterolemia — statin therapy is already recommended regardless of the CAC score
- Very low-risk individuals where the test result is unlikely to change the clinical approach
- Most people under 40, since calcified plaques are uncommon at younger ages
The key principle here is clinical utility: the test is most valuable when there’s genuine uncertainty about treatment, and it can tip the scales meaningfully in one direction.
Conclusion
The CAC scan is not intended as routine screening for the general population. Think of it as a tie-breaker in a conversation between you and your doctor — a tool to sharpen risk assessment when standard measures leave things genuinely unclear.
Used in the right context, it can prevent over-treatment (starting statins in someone whose risk is actually low) and under-treatment (deferring statins in someone who is silently accumulating significant plaque).
If you’re between 40 and 75, have a moderate level of cardiovascular risk, and your doctor is uncertain whether to start or hold off on preventive medications, it may be worth asking whether a CAC scan is appropriate for you.
Related: Chronic Conditions Screening
References:
- Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA Guideline on the Primary Prevention of Cardiovascular Disease. Journal of the American College of Cardiology. 2019.
- Walter KL. What Is a Cardiac CT Calcium Score? JAMA. 2025.
- Golub IS, Termeie OG, Kristo S, et al. Major Global Coronary Artery Calcium Guidelines. JACC: Cardiovascular Imaging. 2023.
- Dzaye O, Razavi AC, Dardari ZA, et al. Modeling the Recommended Age for Initiating Coronary Artery Calcium Testing Among at-Risk Young Adults. Journal of the American College of Cardiology. 2021.
- Greenland P, Blaha MJ, Budoff MJ, Erbel R, Watson KE. Coronary Calcium Score and Cardiovascular Risk. Journal of the American College of Cardiology. 2018.
- Grundy SM, Stone NJ. Coronary Artery Calcium: Where Do We Stand After Over 3 Decades? The American Journal of Medicine. 2021.
- van der Bijl P, Gulati M, Saraste A, et al. Contemporary, Non-Invasive Imaging Diagnosis of Chronic Coronary Artery Disease. The Lancet. 2025.



Leave a comment